Overview
Historically, health centers have used telehealth to better meet their patients’ needs and overcome persistent clinical workforce shortages. Because health centers are required to offer comprehensive services in areas of high need, many are using telehealth to address geographic, economic, transportation, and linguistic barriers to health care access.
During the COVID-19 pandemic, health centers dramatically adopted and increased their use of telehealth. Nearly 95 percent of health centers provided visits virtually. During the Public Health Emergency, Medicare and Medicaid adopted policies which have allowed health centers to provide vital primary and preventive care virtually. These policies allow health centers to ensure their patients continue to receive the care that they rely on, often from the comfort and safety of their own homes.
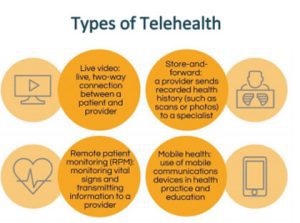
Telehealth Policy Issues
During the COVID-19 pandemic, the Medicare program and state Medicaid agencies adopted more lenient telehealth policies to ensure that patients would have access to critical health care services. For health centers this means:
- Allowing health centers to provide services as distant site providers in the Medicare and Medicaid programs
- Waiving geographic requirements for health centers serving as originating sites and allowing patients to receive care directly from their homes
- Allowing health centers to provide audio-only services in Medicare and in certain states
- Easing HIPAA requirements to allow for providers to use new technologies to communicate with their patients via telehealth
Medicare and Telehealth
For health centers to be able to provide telehealth services in Medicare and be reimbursed for doing so, Congress needed to act. Congress quickly acted at the start of the pandemic, first waiving the geographic restrictions for originating sites (or where the patient is located), allowing broader use of telehealth originating sites, including one’s home. Soon after, Congress gave health centers the authority to serve as distant sites (or where the provider is located) in Medicare for the duration of the public health emergency. However, the payment for these services, as required by law and later determined through guidance from CMS, is $92.03. CMS determined this payment rate is the national average for comparable telehealth services under the Medicare Physician Fee Schedule.
NACHC supports allowing health centers to permanently serve as distant sites in Medicare and at a payment amount that is equal to an in-person visit. There are several legislative efforts in Congress currently to address one or both issues.
Medicaid and Telehealth
The CMS gives states great flexibility in how to cover telehealth (or not) and how it decides to cover and pay for telehealth services in its Medicaid program. This flexibility existed prior to the COVID-19 pandemic and CMS emphasized this flexibility during the pandemic. During the pandemic, all 50 states, plus the District of Columbia and Puerto Rico adopted telehealth policies, with the majority of states paying health centers as they would for in-person visits. Many states also adopted audio-only policies, although reimbursement for those services varied.
NACHC supports state policies that allow health centers to provide telehealth services and reimbursement that is equal to an in-person visit.
Important Links
Center for Connected Health Policy
Telehealth Resources Centers
Centers for Medicare and Medicaid Services Fact Sheet on Telehealth





